WARNING: TORSADES DE POINTES AND SUDDEN DEATH
- Cases of Torsades de Pointes, cardiac arrest, and death have been reported with the use of a higher than recommended dosage of Imocine capsules.
- Imocine are contraindicated in pediatric patients less than 4 years of age.
- Avoid imocine capsules dosages higher than recommended in adults and pediatric patients.
4 years of age and older due to the risk of serious cardiac adverse reactions.
MECHANISM OF ACTION:
In vitro and animal studies show that Loperamide act by slowing intestinal motility and by affecting water and electrolyte movement through the bowel. Loperamide prolongs the transit time of the intestinal contents. It reduces the daily fecal volume, increases the viscosity and bulk density, and diminishes the loss of fluid and electrolytes. PHARMACOKINETICS:
Plasma levels of unchanged drug remain below 2 nanograms per mL after the intake of a 2 mg Loperamide capsule .Plasma Loperamide concentrations are highest approximately 5 hours after administration of the capsule. The peak plasma concentrations of Loperamide were similar for both formulations. The apparent elimination half-life Loperamide in man is about 11 hours with a range of (9-14) hours. The plasma protein binding of Loperamide is about 95%.Elimination of Loperamide mainly occurs by oxidative N-demethylation. Imocine is metabolized mainly by cytochrome P450 (CYP450) isoenzymes. Excretion of the unchanged Loperamide and its metabolites mainly occurs through the feces.
INDICATIONS:
Imocine are indicated for the control and symptomatic relief of acute nonspecific diarrhea in patients 4 years of age and older and of chronic diarrhea in adults associated with inflammatory bowel disease. Imocine are also indicated for reducing the volume of discharge from ileostomies.
CONTRAINDICATIONS:
Pediatric patients less than 4 years of age.
Patients with a known hypersensitivity to Imocine or to any of the excipients.
Patients with abdominal pain in the absence of diarrhea.
Patients with acute dysentery, which is characterized by blood in stools and high fever.
Patients with acute ulcerative colitis.
Patients with bacterial enterocolitis caused by invasive organisms including Salmonella, Shigella, and Campylobacter.
Patients with pseudomembranous colitis (e.g. Clostridium difficle) associated with the use of broad-spectrum antibiotics.
WARNINGS & PRECAUTIONS:
- The use of Imocine does not preclude the need for appropriate fluid and electrolyte therapy in patients who have diarrhea especially young children.
- Imocine must be discontinued promptly when constipation, abdominal distention or ileus develop.
- Treatment of diarrhea with Imocine is only symptomatic. Whenever an underlying etiology can be determined, specific treatment should be given when appropriate (or when indicated).
- Imocine should be used with special caution in young children because of the greater variability of response in this age group. Dehydration, particularly in younger children, may further influence the variability of response to imocine.
- Extremely rare allergic reactions including anaphylaxis and anaphylactic shock have been reported.
- In acute diarrhea, if clinical improvement is not observed in 48 hours, the administration of Imocine should be discontinued and patients should be advised to consult their physician.
- Patients with AIDS treated with Imocine capsules for diarrhea should have therapy stopped at the earliest signs of abdominal distention. There have been isolated reports of toxic megacolon in AIDS patients with infectious colitis from both viral and bacterial pathogens treated with Imocine.
- Cardiac events including QT prolongation and torsades de pointes have been reported in association with overdose.
- Imocine should not be used when inhibition of peristalsis is to be avoided due to the possible risk of significant sequelae including ileus, megacolon and toxic megacolon. Imocine must be discontinued promptly when constipation, abdominal distention or ileus develop.
Hepatic Impairment: Imocine should be used with caution in patients with hepatic impairment, because of reduced first pass metabolism.
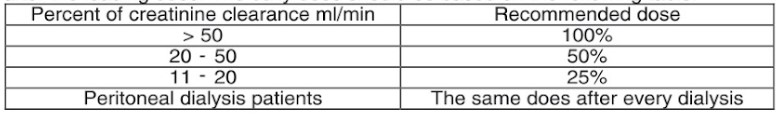
Renal Impairment: dosage adjustments in patients with renal impairment are not required
Pregnancy (Category C):
Imocineshould be used during pregnancy only if the potential benefit justifies the potential risk to the fetus. It is not advisable to administer IMOCINE in pregnancy, especially during the first trimester.
Nursing Mothers Small amounts of imocine may appear in human breast milk. Therefore, Imocine is not recommended during breast-feeding.
Effects on ability to drive and use machines:
Loss of consciousness, depressed level of consciousness, tiredness, dizziness, or drowsiness may occur when diarrhea is treated with Loperamide. Therefore, it is advisable to use caution when driving a car or operating machinery.
DRUG INTERACTIONS:
Concomitant use of Imocine capsules with inhibitors of CYP3A4 (e.g., itraconazole) or CYP2C8 (e.g., gemfibrozil) or inhibitors of P-glycoprotein (e.g., quinidine, ritonavir) can increase exposure to Loperamide. The increased systemic exposure to Imocinemay increase a risk for cardiac adverse reactions especially in patients who are taking multiple CYP enzyme inhibitors, or in patients with underlying cardiac conditions. Monitor patients for cardiac adverse
reactions.
When imocine capsules are given with saquinavir, the therapeutic efficacy of saquinavir should be closely monitored. Combination with others drugs or herbal products that are known to prolong the QT interval, including:
Class 1A (e.g., quinidine, procainamide) or Class III (e.g., amiodarone, sotalol)
Antiarrhythmic, antipsychotics (e.g., chlorpromazine, haloperidol, thioridazine, ziprasidone),
Antibiotics (e.g., moxifloxacin), or any other drug known to prolong the QT interval (e.g., pentamidine, levomethadyl acetate, methadone) should be avoided.
SIDE EFFECTS:
The most common side effects: Headache, Dizziness, Constipation, Nausea, Flatulence.
Uncommon: Somnolence, Abdominal pain, abdominal discomfort, Dry mouth, Abdominal pain upper, Vomiting, Dyspepsia, rash.
DOSAGE & ADMINISTRATION:
Patients should receive appropriate fluid and electrolyte replacement as needed.
- Acute Diarrhea:
Adults: The recommended initial dose is 4 mg (two capsules) followed by 2 mg (one capsule) after each unformed stool. Daily dosage should not exceed 16 mg (eight capsules). Clinical improvement is usually observed within 48 hours.
Children: For children 4 to 12 years of age, the following schedule for capsules will usually fulfill initial dosage requirements.
Recommended First Day Dosage Schedule:
4 to five years (15 to 20 kg): 1 mg t.i.d. (3 mg daily dose).
Six to eight years (20 to 30 kg): 2 mg b.i.d. (4 mg daily dose).
Eight to twelve years (greater than 30 kg): 2 mg t.i.d. (6 mg daily dose).
Recommended Subsequent Daily Dosage:
Following the first treatment day, it is recommended that subsequent Imocine doses (1 mg/10 kg body weight) be administered only after a loose stool. Total daily dosage should not exceed recommended dosages for the first day. Children under 4 Years: The use of Imocine in children under 4 years is not recommended.
- Chronic Diarrhea:
Adults: The recommended initial dose is 4 mg (two capsules) followed by 2 mg (one capsule) after each unformed stool until diarrhea is controlled, after which the dosage of Imocine capsules should be reduced to meet individual requirements. When the optimal daily dosage has been established, this amount may then be administered as a single dose or in divided doses
Children Under 4 Years: The use of Imocine in children under 4 years is not recommended. OVERDOSE:
Symptoms: In cases of overdose, (including relative overdose due to hepatic dysfunction), urinary retention, paralytic ileus and CNS depression may occur. Children may be more sensitive to CNS effects than adults.
In individuals who have ingested overdoses of Imocine HCI, cardiac events such as QT interval prolongation, torsades de pointes, other serious ventricular arrhythmias, cardiac arrest and syncope have been observed .Fatal cases have also been reported.
Treatment: If symptoms of overdose occur, naloxone can be given as an antidote. Since the duration of action of imocineis longer than that of naloxone (1 to 3 hours), repeated treatment with naloxone might be indicated. Therefore, the patient should be monitored closely for at least 48 hours in order to detect possible CNS depression.
PACKAGING:
1 blister contains 10 Imocine capsules/carton box.
STORAGE CONDITIONS:
Store in cool and dry place below 25 °C. – Keep out of reach of children.